Date: 26 May 2016
Copyright: n/a
Notes:
Obituary written on ISHAM website:
December 21, 1941- March 2, 2016
It is with deep sadness that we announce that Ira F. Salkin, PhD died on March 2, 2016 having lost his long battle with COPD and congestive heart failure. His passing is a great loss to the community of medical mycology. Born in Chicago, Ira attended Northwestern University for both his Bachelors and Master degrees (1959-1964) prior to moving west to earn his PhD in 1969 from the University of California, Berkeley. Ira began a long career in mycology with his doctoral work, where he used his NSF pre-doctoral award to study the biology of aquatic fungi. Upon completion of his PhD he moved east to Albany New York where he spent the next 32 years with the New York State Department of Health in the Wadsworth Laboratories, later to become a Director of numerous State laboratories and programs. These included the Medical Mycology Laboratories, Clinical Laboratory Approval Program, Biological Safety, Medical Waste and Quality Control. During his career he published more than 120 articles in peer-reviewed journal and chapters in textbooks.
Ira was deeply involved in several scientific societies and was recognized by his peers for his energetic efforts in these societies. He was a long-standing member the American Society for Microbiology, was the Chair of Division F in 1990-91 and was elected as a Fellow of the American Academy of Microbiology. He received the Lippmann Award for Scientific Achievement of the Medical Mycology Society of New York. In 1991, Ira was awarded the Billy H. Cooper award from the Medical Mycology Society of the Americas in recognition of his efforts in clinical mycology, as well as the Meridian Award. In 2015, Ira was granted the Distinguished Service award by ISHAM, which speaks for itself.
Ira’s great passion was scientific publication ranging from the ethics of publication to journal editing, which amounted to possibly some of his greatest contributions Over the last 25 years Ira served as an Editor of the Journal of Clinical Microbiology from 1990-2000, the Editor-in-Chief of the Journal of Applied Biosafety from 2001-2004, and from 2004 through 2015 he was the Editor-in-Chief of Medical Mycology. This also made him an ex officio member of the Council of ISHAM. As part of his efforts for Medical Mycology he organized very popular sessions at three separate ISHAM congresses directed toward young scientists on how to write and publish a scientific paper. His speaking style and wit, intermingled with his pearls of publishing and writing wisdom, were always well received. He was a very difficult act to follow especially if you were the next speaker. His efforts as the Editor in Chief of ISHAM’s own journal, Medical Mycology, were unparalleled as he raised the visibility and impact of the journal but also improved the quality of many articles as copy editor and even smoothed the grammar of the accepted manuscripts. This may not always have been received well but most authors were very pleased once they saw their work in press. As relayed to us by his loving wife Kay, “Ira was always happiest when sitting at his computer working on a manuscript”.
For those of us privileged to know Ira well, he was a man with a very quick, dry wit, had an eager willingness to “argue” a point aggressively without hostility and was someone who had vast life experience, which he was willing to share especially over a night cap of a good malt uisge beatha or “water of life” of Scottish provenance. His liberal views in politics and other areas, possibly a holdover from his days in Berkeley in the ‘60’s, guided these discussions. Ira enjoyed many informal symposia i.e., a fine meal and libation during which he and his companions solved many of the problems of the world. Ira was a good colleague and a great friend to many and selflessly put others ahead of himself. He was indeed a scholar and a gentleman. Those of us who counted Ira a friend will miss him greatly. The Medical Mycology community has also lost one of its shining beacons.
Ira is survived by his devoted wife, Kay (Brown) Salkin; stepdaughters, Lori Hewig and Beth (Gerard) Weir; stepson, William (Tracy) Schwarz; son, Daniel; and grandchildren, Lindsay and Elise Weir, and Benjamin and Cameran Schwarz. Ira was pre-deceased by parents, Irving and Mollie Salkin, and brother, Marshall Salkin.
We invite anyone wishing to relate a story concerning Ira to send it to the ISHAM website for inclusion in this tribute to an important member of the Medical Mycology community.
Karl V. Clemons, Chester R. Cooper, J. Peter Donnelly
April, 2016
Images library
-
Title
Legend
-
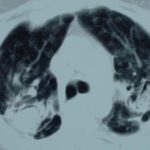
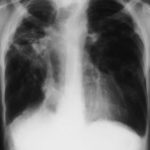
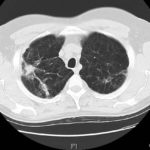
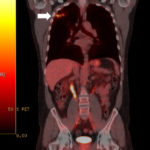
This 54 year old man developed right upper lobe shadowing after development of cough, chest pain and shortness of breath. He suffered from emphysema. Investigations, including a PET scan suggested carcinoma of the lung. He underwent an apical resection and histology showed bullae in the lung with one containing necrotic material and conidial heads consistent with Aspergillus.
Histology:
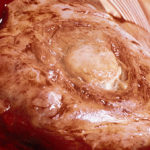
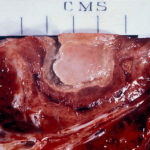
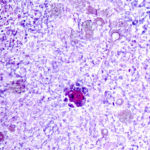
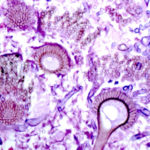
Two wedges of lung tissue were examined. The larger 90 x 35 x 35mm with adherent parietal pleura 100 x 45mm. Sectioning reveals irregular scarring and bullae in the lung tissue. No definite tumour is identified. A focus of possible necrosis up to 10mm in diameter is present, 10mm from the pleura and 20mm from the nearest staple line. Lung and adherent parietal pleura show dense fibrosis around a cavity (see fig A) arrow, lined by granulation tissue and fibrin. This is filled with necrotic material (Fig B) and branching septate fungal hyphae with conidial heads, consistent with Aspergillus and a fungal ball.(Fig C at higher power). A few scattered granulomata are seen away from the cavity. No invasion of lung parenchyma was seen. There is congestion of the lung parenchyma and collections of pigmented macrophages are seen within air spaces.Legends:
A- Section of lung showing a fungal ball within a cavity (x25). B- Showing branching septate hyphae with conidial heads (x250) C- Higher power magnification (x 500) showing the conidial heads more clearly. D – Edge of cavity showing from left to right – necrosis, granulaomatous reaction, fibrosis, chronic inflammation (x100). E- CT scan (July 08) showing a speculated nodular lesion in the right apex. F – Chest X-ray (May 08) – showing right upper lobe shadowing. G.PET scan (July 08)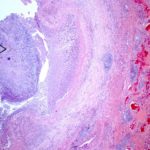 ,
,  ,
,  ,
,  ,
,  ,
,  ,
, 
-
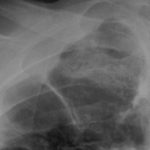
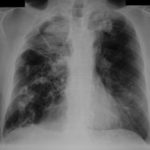
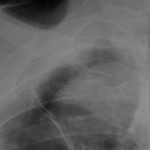
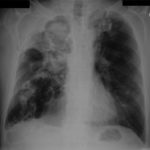
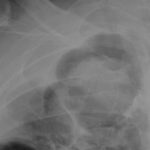
Pt DB This patient with longstanding pulmonary disease developed Mycobacterium avium pulmonary infection which was treated. X rays in Jan 05 through to May 06 revealed an aspergilloma in upper right lobe cavity. Following a severe prolonged bout of coughing up black material- X rays on 22/9/07 showed a disappearance of the aspergilloma.( Images G & H). Go to case history
 ,
,  ,
,  ,
,  ,
,  ,
,  ,
,  ,
, 
-
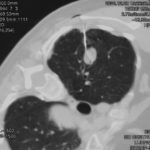
This 63 year old smoker presented with a new small mass in the right upper lobe. She had had tuberculosis as a teenager (1958) which recurred in 1962, requiring 2 long stays in a sanatorium. Since then she was well, until a new shadow was noticed on her chest X-ray. A CT showed a smooth round nodule, and to rule out carcinoma it was biopsied percutaneously. Histology showed fungal hyphae, consistent with Aspergillus , and serology confirmed infection with Aspergillus fumigatus. Following biopsy, an air fluid pocket has appeared, most consistent with an aspergilloma, as the lesion is solitary.
-
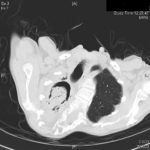
Patient MD with kyphoscoliosis and chronic cavitary pulmonary aspergillosis and an aspergilloma. Patient exhibited azole resistant A. fumigatus.
Further details
Image A. This CT scan cut shown shows a grossly distorted thorax because of the kyphoscoliosis, a nearly normal appearing left lung, her trachea at an odd angle, demonstrating the normal cartilage rings and an aspergilloma in a cavity which has replaced the right upper lobe. The cavity is surrounded by significant pleural thickening and fibrosis.
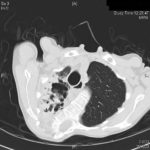
Image B. The other cut (slightly inferior) shows a complex large cavity and some smaller ones posteriorly, with some material consistent with a fungal ball within the large cavity. There is a separate cavity anteriorly and small air spaces within the extensive pleural thickening. Her trachea is widened. the left lung appears normal.
This patient with repaired juvenile scoliosis first recognised that she had pulmonary aspergillosis when she coughed up large amounts of blood, she was admitted to ICU and underwent bronchial artery embolisation, followed by tranexamic acid orally. A. fumigatus was cultured from sputum. A diagnosis of chronic cavitary pulmonary aspergillosis with an aspergilloma was made. She didn’t improve with itraconazole (no fall in Aspergillus precipitins and continuing symptoms, despite good blood levels) and was treated with voriconazole. She had a good sympomatic response, with marginal improvement in her Aspergillus precipitins titre. Remission continued for over 3 years but then her symptoms of cough and general fatigue returned. Her sputum grew A. fumigatus again, which had MICs to itraconazole (>8 mg/L, resistant), voriconazole (8mg/L, resistant) and posaconazole (2mg/mL, resistant). She is being treated with amphotericin B.
 ,
, 
-
Histopathological appearance of a fungus ball: it consists of a tangled mass of branching, septate hyphal with vesicular swellings in the center (H&E, x 200).

-
Further image details
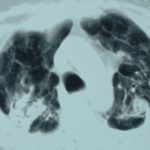
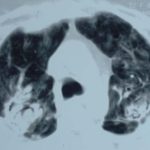
Image A. Long standing sarcoidosis, on corticosteroids with fibrosis and cavitary disease, and a possible fungal ball in the cavity on the left (1996).
Image B. Long standing sarcoidosis, on corticosteroids with 2 cavities containing aspergillomas, one on the left and one on the right (1996).
Image C. Sarcoidosis with progressive cavity formation and aspergillomas. Probable CIPA given appearances (2000).
Image D. Sarcoidosis with progressive cavity formation and aspergillomas. Probable CIPA given appearances (2000).
Image E. Sarcoidosis with progressive cavity formation and aspergillomas. Probable CIPA given appearances (2000).
 ,
,  ,
,  ,
,  ,
,