Date: 26 November 2013
Aspergillus terreus Thom. Conidial head of Aspergillus terreus. Conidial heads are compact, columnar and biseriate. Conidiophores are hyaline to slightly yellow and smooth walled.
Copyright:
With thanks to G Kaminski. D Ellis and R Hermanis Mycology Unit, Women’s & Children’s Hospital , Adelaide, South Australia 5006
Notes:
Colonies on CYA 40-50 mm diam, plane, low and velutinous, usually quite dense; mycelium white; conidial production heavy, brown (Dark Blonde to Camel, 5-6D4); reverse pale to dull brown or yellow brown. Colonies on MEA 40-60 mm diam, similar to those on CYA or less dense. Colonies on G25N 18-22 mm diam, plane or irregularly wrinkled, low and sparse; conidial production light, pale brown; brown soluble pigment sometimes produced; reverse brown. No growth at 5°C. Colonies at 37°C growing very rapidly, 50 mm or more diam, of similar appearance to those on CYA at 25°C.Conidiophores borne from surface hyphae, stipes 100-250 μm long, smooth walled; vesicles 15-20 μm diam, fertile over the upper hemisphere, with densely packed, short, narrow metulae and phialides, both 5-8 μm long; conidia spherical, very small, 1.8-2.5 μm diam, smooth walled, at maturity borne in long, well defined columns.Distinctive featuresVelutinous colonies formed at both 25°C and 37°C, uniformly brown, with no other colouration, and minute conidia borne in long columns make Aspergillus terreus a distinctive species.
Images library
-
Title
Legend
-
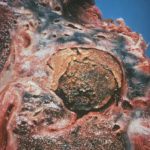
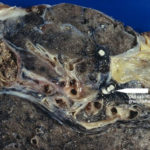
Macroscopic view medial aspect of left upper lobe of lung showing segmental collapse and congestion of lower segments, with mucus extruding from incised bronchi.
 ,
,  ,
,  ,
,  ,
, 
-
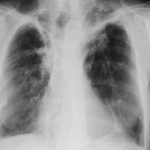
Born 75 years ago, Pt HK had 3 episodes of tuberculosis as a child and teenager, being treated with PAS and streptomycin. He suffered a ‘bad chest’ all his life and retired aged 54. Presenting with worsening and more frequent chest infections, he was referred with ‘bronchiectasis and Aspergillus sensitisation’. A diagnosis of chronic pulmonary aspergillosis was made in June 2009 on the basis of his chest radiograph and strongly positive Aspergillus precipitins (IgG antibodies) (titre 1/16). He also had Pseudomonas aeruginosa colonisation. His oxygen saturation was 87% and his pO2 6.8, pCO2 6.2 KPa.
His chest radiograph (see above, November 2009) was reported as showing; “ The lung fields are over-inflated. Bilateral apical fibrotic change secondary to old TB. No cavity seen.” At clinic, bilateral apical cavities were seen, with some associated pleural thickening at the left apex, without any evidence of a fungal ball.
He started posaconazole 400mg twice daily with therapeutic levels at subsequent visits. Sputum cultures never grew Aspergillus. Over the following 9 months he had no chest infections requiring antibiotics, his breathlessness worsened gradually and he remained easily fatigued. His Aspergillus antibody titres fell. Overall he felt better, but was concerned about declining respiratory status.